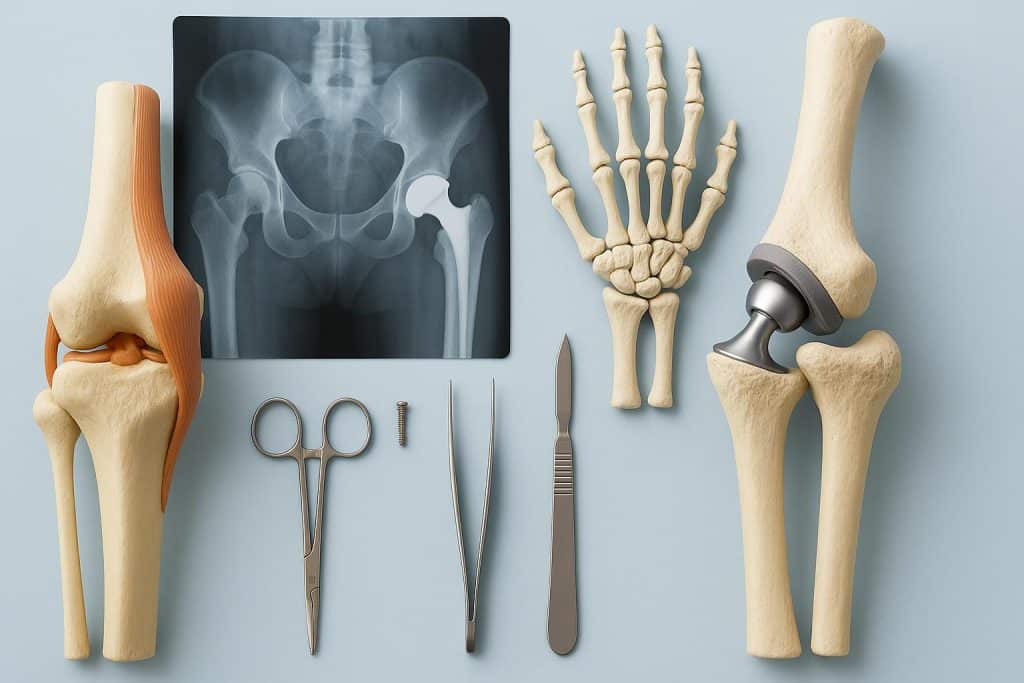
The Art and Science of Bone & Joint Surgery
What Makes Bone & Joint Surgeons Unique?
Bone and joint surgeons, commonly referred to as orthopedic surgeons, represent a distinctive combination of precision, artistry, and scientific knowledge. These bone & joint surgeons specialize in diagnosing, treating, and rehabilitating conditions affecting the musculoskeletal system, including bones, joints, ligaments, tendons, and muscles. What distinguishes them from other medical professionals is their extensive training, which includes medical school, a surgical residency, and often additional fellowships in subspecialties such as sports medicine, joint replacement, or pediatric orthopedics. This demanding educational path equips bone & joint surgeons with exceptional surgical skills while also providing a deep understanding of human anatomy, biomechanics, and the underlying causes of musculoskeletal disorders.
Furthermore, the complexity of the procedures performed by bone & joint surgeons requires a comprehensive and patient-focused approach to care. They must be highly skilled in minimally invasive techniques, enabling them to carry out procedures through small incisions while minimizing damage to surrounding tissues. This approach not only shortens recovery time but also lowers the risk of complications, demonstrating how bone & joint surgeons effectively merge technical expertise with sound clinical judgment and compassionate care. Ultimately, the strength of bone & joint surgeons lies not only in their surgical precision but also in their dedication to promoting long-term patient health through education, rehabilitation, and preventive strategies.
The Evolution of Techniques in Musculoskeletal Surgery
The field of orthopedics has seen remarkable advancements over the past few decades, transforming how conditions affecting bones and joints are managed. Traditionally, orthopedic surgery was largely dependent on open surgical techniques, with significant incisions and longer recovery times. However, the advent of arthroscopy, a minimally invasive surgery technique has revolutionized the field. This technique allows surgeons to visualize and operate on the interior of joints through small incisions using a camera and specialized instruments. As a result, patients benefit from less pain, shorter hospital stays, and quicker return to their daily lives.
Moreover, recent developments in the use of robotics and computer navigation systems have enhanced precision during surgical procedures. Surgeons can now perform complex joint reconstructions or replacements with unparalleled accuracy. These technological advancements are not merely trends; they represent a paradigm shift within orthopedic surgery that continues to evolve with ongoing research and innovation. Techniques such as 3D printing are paving the way for personalized implants that fit the unique anatomy of each patient, further enhancing the success rate of procedures.
How Technology is Transforming Surgical Practices
The integration of technology in orthopedic surgery is exponentially improving outcomes and patient experiences. One significant incorporation is in the realm of telemedicine. With the growing demand for accessible health services, orthopedic surgeons are utilizing telehealth platforms to conduct pre-operative assessments, post-operative follow-ups, and even physical therapy sessions. This approach not only saves time and resources but also increases accessibility for patients who may reside in rural areas or have mobility challenges.
Alongside telemedicine, advancements in imaging technology, such as MRI (Magnetic Resonance Imaging) and CT (Computed Tomography) scans, allow for precise diagnostics, so surgeons can devise the most effective treatment plans tailored to the individual. Furthermore, the ongoing development of mobile health applications helps patients engage with their treatment regimens and provides educational resources at their fingertips. This shift toward incorporating technology into surgical practice is not only enhancing the surgical experience but is also leading to improved patient education and empowerment, contributing to better overall outcomes.
Common Conditions Treated by Bone & Joint Surgeons
Unpacking Arthritis: More Than Just Joint Pain
Arthritis represents one of the most prevalent conditions that bone and joint surgeons encounter. Often misconceived as merely the natural deterioration of joints with age, arthritis encompasses over 100 different types, aching not just the elderly but individuals of all ages. Conditions such as osteoarthritis, rheumatoid arthritis, and juvenile idiopathic arthritis can lead to debilitating pain, swelling, stiffness, and reduced mobility. Unfortunately, for many, these symptoms can severely affect one’s quality of life, prompting the need for surgical intervention in advanced stages.
Bone and joint surgeons are pivotal in diagnosing arthritis and developing comprehensive treatment plans that often start with conservative management, including medications, physical therapy, and lifestyle modifications. However, when these approaches fail, surgical options ranging from arthroscopy to joint replacement may become necessary. The latter involves removing the damaged joint surface and replacing it with prosthetic components. While surgery can provide substantial relief and restore function, ongoing research into biologic therapies, such as stem cells and PRP (Platelet-Rich Plasma) injections, is promising for treating arthritis without invasive measures. These innovative treatments may help preserve existing joints and offer hope to those who seek alternatives to traditional surgery.
Fractures and Trauma: The Surgeon's Quick Response
Fractures and traumatic injuries represent another domain where bone and joint surgeons' expertise is crucial. Whether they result from high-impact sports activities, falls, or accidents, fractures can vary dramatically in severity from simple hairline fractures that might require little more than rest, to complex fractures involving multiple broken bones requiring extensive surgical reconstruction. Bone and joint surgeons are trained to respond rapidly to traumatic injuries, often being part of multidisciplinary teams in emergency rooms to provide immediate care that could save limbs or even lives.
The effective management of trauma often involves advanced imaging studies to assess the extent of injury, followed by a tailored surgical approach that can include stabilization with plates, screws, or external fixators. In the case of displaced fractures where bones are misaligned, precise surgical realignment is critical to restore function and prevent long-term complications. Post-operative care and rehabilitation play an equally important role, with bone and joint surgeons closely coordinating with physical therapists to ensure that patients regain strength and mobility as quickly and safely as possible.
From Sports Injuries to Everyday Aches: When to Seek Help
Another area of focus for bone and joint surgeons lies in sports injuries and general musculoskeletal pain conditions often overlooked until they become debilitating. Sports-related injuries, such as ligament tears, tendonitis, or bursitis, can occur unexpectedly and may require urgent medical attention. Yet, even less dramatic complaints, like ongoing joint pain or discomfort, should not be ignored. These symptoms could signify underlying issues such as tendinopathy or stress fractures that, if left untreated, might evolve into more severe conditions.
Bone and joint surgeons emphasize the importance of understanding the body's signals, encouraging individuals to seek early intervention when experiencing persistent pain, even if it seems mild at first. With the right diagnosis and treatment, many patients can return to their activities, whether competitive sports or day-to-day tasks, with optimal function. This proactive approach bolsters the idea that musculoskeletal health is not just for athletes but is essential for everyone, fostering a culture of preventive care and timely surgical intervention when necessary.
Patient Experience and Expectations: What to Know
The Consultation Process: A Closer Look
The consultation process is a cornerstone of patient experience in orthopedic care. This initial meeting serves as the foundation for understanding the patient’s history, current symptoms, and their impact on daily life. During this appointment, a bone and joint surgeon will perform a comprehensive evaluation, including a detailed physical examination and review of any existing imaging studies (like X-rays or MRIs). Patients should come prepared to discuss their medical history, lifestyle, and any specific concerns they might have, as an open dialogue is vital to tailoring an effective treatment plan.
It’s important for patients to feel comfortable expressing their expectations and desired outcomes from treatment during this phase. Policies emphasizing shared decision-making have begun to reshape how surgeons engage with their patients, allowing for a more collaborative approach. Surgeons now strive to educate patients about their specific conditions, various treatment options, and the implications of each choice, empowering individuals to make informed decisions about their care. This not only reinforces trust but also encourages patients to take an active role in their recovery journey.
Understanding Surgical Options and Outcomes
Once a diagnosis has been established, the next stage involves discussing potential surgical options, each of which carries implications for recovery and rehabilitation. Patients often find themselves grappling with the decision between conservative management versus surgery, and understanding the potential outcomes of either choice is critical. Bone and joint surgeons utilize evidence-based practices to guide their recommendations, explaining risks, benefits, and expected recovery timelines associated with each surgical intervention. Common procedures like arthroscopy, joint replacement, or spinal surgery can vary significantly in their invasiveness and postoperative care requirements.
Outcomes are influenced by various factors, including the patient’s age, overall health, and adherence to rehabilitation protocols post-surgery. Thus, surgeons highlight the importance of realistic expectations and emphasize that successful outcomes not only depend on surgical technique but also on the patient’s commitment to the comprehensive recovery plan. This thorough understanding fosters not only trust in the surgical team but also encourages a sense of ownership of one’s health journey.
Rehabilitation: The Bridge to Recovery
Rehabilitation is often regarded as the unsung hero of orthopedic outcomes, serving as the crucial bridge between surgery and full recovery. Once an orthopedic surgery is performed, the body enters a healing phase requiring strategic rehabilitation to restore function and adaptability. A well-structured rehabilitation program is tailored to each patient’s specific procedure, medical history, and physical capabilities. Bone and joint surgeons frequently collaborate with physical therapists to develop individualized recovery plans that focus on regaining range of motion, strength, and overall mobility.
Moreover, it is essential for patients to understand the timeline for recovery and the importance of adhering to their rehabilitation program. Challenges during the recovery process are not uncommon; however, maintaining open communication with both the surgeon and rehabilitation team can help navigate these challenges effectively. The ultimate goal transcends beyond healing; it involves enabling patients to return to their desired level of physical activity, whether that means returning to competitive sports, enjoying family activities, or performing daily tasks without discomfort.
The Future of Orthopedic Surgery: Trends to Watch
Regenerative Medicine: Healing Beyond Traditional Surgery
The next frontier in orthopedic surgery might just lie within the field of regenerative medicine. This innovative approach aims to harness the body’s intrinsic healing capabilities, offering alternative solutions to injuries and degenerative conditions. Regenerative treatments, including stem cell therapy and tissue engineering, represent a significant departure from traditional surgical techniques, focusing on regeneration rather than just repair. By using the body’s own cells, like those harvested from bone marrow or fat tissue, surgeons hope to stimulate healing processes in damaged tendons, ligaments, or cartilage.
Research in this area is advancing quickly, providing promising outcomes for conditions previously deemed untreatable without invasive surgery. Early studies indicate that patients receiving regenerative treatments may experience significant improvements in pain reduction and function, potentially prolonging joint integrity and postponing the need for conventional surgeries, such as joint replacements. As regenerative medicine continues to evolve, it holds the potential to fundamentally reshape the orthopedic landscape, offering patients more options and pathways to recovery than ever before.
Personalized Treatments: Tailoring Care for Every Patient
In modern medicine, the concept of personalized treatment is gaining traction, and orthopedic surgery is no exception. Bone and joint surgeons are increasingly recognizing that every patient’s condition is unique, which calls for an individualized approach to treatment. This personalization can manifest in various ways in surgical technique, selection of implants, and rehabilitation strategies. By closely analyzing patient demographics, condition severity, and personal health history, orthopedic surgeons can tailor their treatment plans to optimize outcomes.
Furthermore, the increasing availability of genomic testing and biomarkers may revolutionize how surgeons assess risks and choose therapies. Studies suggest that certain genetic markers could predict individual responses to surgical interventions or rehabilitation protocols. As such, the move towards personalized treatments not only enhances the quality of care but fosters deeper patient engagement, as individuals come to appreciate their unique treatment journey.
Artificial Intelligence in Bone & Joint Care: A Game Changer?
Artificial intelligence (AI) stands on the precipice of transforming the orthopedic landscape, promising enhanced precision in diagnostics and treatment planning. From predictive analytics that help foresee potential complications to AI-powered imaging technologies that can identify fractures or degenerative changes at unprecedented levels of accuracy, the possibilities are vast. Machine learning algorithms can analyze vast datasets from previous patients to optimize surgical strategies and predict outcomes, a helpful tool for bone and joint surgeons striving for the best possible care for their patients.
AI also plays a critical role in streamlining patient management through advanced tracking systems. These digital platforms can track patient recovery in real-time, offering both surgeons and patients immediate feedback regarding progress and areas needing attention. As AI continues to develop, it is likely to occupy an ever-expanding role in the orthopedics field, potentially enhancing the accuracy of operations while allowing surgeons to focus more intently on complex aspects of patient care.
Angela Spearman is a journalist at EzineMark who enjoys writing about the latest trending technology and business news.